Lead poisoning in India
UNICEF and Pure Earth's 2020 report reveals that a significant percentage of children in India are afflicted with high blood lead levels. Specifically, approximately half of the children are affected.
Major findings
High Blood Lead Levels
- 275 million children in India have blood lead levels beyond the tolerable limit of 5 µg/dL.
- 64.3 million children's blood lead levels exceed 10 µg/dL.
- 23 states exceed the 5 µg/dL margin.
Disability-Adjusted Life Years:
- Lead toxicity in India contributes to 4.6 million Disability-Adjusted Life Years and 165,000 deaths annually.
Adverse Health Impact
- Lead enters the bloodstream and goes directly to the brain.
- Causes anemia and various illnesses affecting neurological, skeletal, and neuromuscular systems.
Challenges to Cope with Lead Poisoning
- Less Attention is given to lead poisoning compared to other public health concerns.
- Poor Recycling Laws - Unscientific techniques are employed during recycling, in an unregulated and uncontrolled way.
- High demand for Cheap Products - People are not willing or able to pay more for lead-free alternatives.
Solutions:
- Regular screening and testing of lead sources.
- Discouraging informal recycling operations and regulating the sector.
- Enhancing testing capacity and creating facilities for blood lead level screenings at every district hospital.
- Devising strategies on a state level, through regional bureaucracy, local press, and vernacular language.
Lead poisoning:
Lead poisoning is a serious health condition that occurs when a person is exposed to high levels of lead. Lead is a toxic heavy metal that can accumulate in the body over time, causing various health problems. This condition is particularly dangerous for children and pregnant women, as it can cause developmental and neurological damage.
Sources of lead poisoning:
Lead can be found in various everyday items, including paint, water, soil, and air. Lead-based paint is the most common source of lead poisoning in children, especially in old homes or buildings that were constructed before the 1970s. Lead can also contaminate water through old pipes, faucets, and fittings, and soil through industrial or environmental pollution.
Symptoms of lead poisoning:
Lead poisoning can cause a wide range of symptoms, including stomach pain, headache, fatigue, irritability, nausea, constipation, and even seizures. Children may experience developmental delays, learning difficulties, and behavioral problems, while pregnant women may suffer from premature delivery, miscarriage, or stillbirth.
Diagnosis and treatment:
Blood tests can be performed to diagnose lead poisoning. The treatment for lead poisoning depends on the severity of the condition. In mild cases, treatment may involve removing the source of lead exposure, while severe cases may require chelation therapy to remove lead from the body.
Prevention:
The best way to prevent lead poisoning is to identify and remove sources of lead exposure. This includes using lead-free paints, drinking water from a safe source, and avoiding contact with soil or dust that may contain lead. It is also important to maintain good hygiene and wash hands frequently, especially before eating.
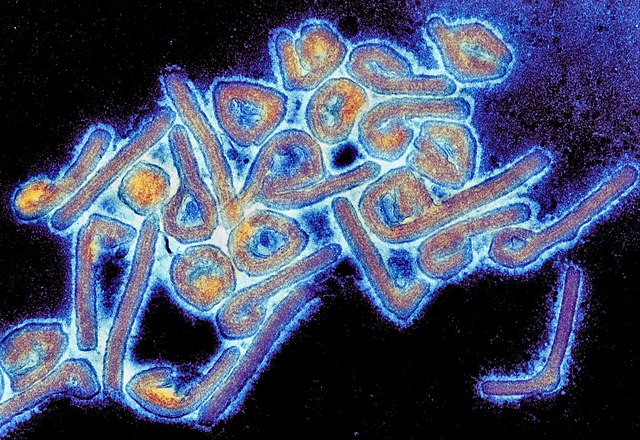
Marburg virus disease
Equatorial Guinea, a Central African country has confirmed its first-ever outbreak of Marburg virus disease.
Marburg virus disease
Marburg virus is a deadly virus that belongs to the family of filoviruses, which also includes the well-known Ebola virus. It was first identified in the city of Marburg, Germany in 1967, where it caused an outbreak among laboratory workers who were exposed to infected monkeys imported from Uganda.
Marburg virus is highly infectious and can cause a severe and often fatal hemorrhagic fever, with symptoms ranging from fever, headache, muscle pain, and vomiting to internal bleeding and organ failure. The virus is transmitted through contact with the bodily fluids of infected people or animals, and there is currently no specific treatment or vaccine available for it.
The virus is primarily found in sub-Saharan Africa, where outbreaks have occurred sporadically since its discovery. The largest recorded outbreak of Marburg virus occurred in Angola in 2005, which resulted in over 400 cases and a mortality rate of around 90%.
Due to its potential for causing severe disease and high mortality rates, Marburg virus is classified as a Category A bioterrorism agent by the United States. This means that it poses a significant threat to public health and national security, and requires special attention and preparedness measures by health authorities and government agencies.
In terms of prevention, the best way to avoid Marburg virus is to avoid contact with infected people or animals. This includes avoiding travel to areas where outbreaks have occurred, wearing protective gear when working with potentially infected materials, and practicing good hygiene habits such as frequent hand washing.
Marburg virus remains a significant public health concern, and continued research into its prevention and treatment is essential for protecting global health security. As with other infectious diseases, early detection, rapid response, and effective communication are critical for limiting the spread of the virus and preventing further outbreaks.
Elephantiasis or Lymphatic Filariasis (LF)
13-Feb-2023: Ministry of Health & Family Welfare launches nationwide Sarva Dawa Sevan or Mass Drug Administration (MDA) campaign to Eliminate Lymphatic Filariasis (LF)
Nationwide Mass Drug Administration Campaign was launched by the Ministry of Health and Family Welfare. India aims to eliminate filariasis by 2027, three years ahead of the global target. High-burdened areas are Bihar, Chhattisgarh, Jharkhand, Maharashtra, Uttar Pradesh, West Bengal, Karnataka, Odisha, Madhya Pradesh and Andhra Pradesh.
Filariasis
- Parasitic infection caused by microscopic, thread-like worms.
- Spread by the bite of infected mosquitoes.
- Affects millions of people in tropical and subtropical regions worldwide.
Causes and Transmission
- Caused by nematodes (roundworms) of the family Filariodidea.
- 3 types of filarial worms: Wuchereria bancrofti, Brugia malayi, and Brugia timori.
Symptoms
- Asymptomatic, acute, and chronic conditions.
- Chronic conditions lead to lymphoedema, elephantiasis, and hydrocele.
Treatment
- WHO recommends three drug treatments to accelerate global elimination of lymphatic filariasis.
- Treatment known as IDA involves a combination of ivermectin, diethylcarbamazine citrate, and albendazole.
- Plan involves administering drugs for two consecutive years.
- Adult worm has a life of only four years and dies a natural death without causing harm to the person.